Introduction
Optimizing care for people between pregnancies is imperative to improving maternal and infant health. This period is referred to as the interpregnancy interval (IPI). The American College of Obstetricians and Gynecologists (ACOG) recommends that IPIs shorter than six months be avoided, and the lowest risks of adverse outcomes, such as preterm birth and low birth weight, are associated with IPIs greater than 18 months.1,2 With adequate time between pregnancies, parents are able to optimize care for their chronic conditions, which may improve both future pregnancy outcomes and maternal health outcomes across the lifespan.3 In North Carolina, in 2018, 12.7% of pregnancies had an IPI of < 6 months.4
One way to reduce the number of unintended pregnancies and short IPIs is through contraception. Long-acting reversible contraceptives (LARC) are the most effective reversible contraception methods available and have high continuation rates and patient satisfaction. LARC come in two main forms: intrauterine devices (IUDs), which can be either hormonal or non-hormonal, and the contraceptive hormonal implant. Benefits to these devices include their high effectiveness, ease of use, and quick return to baseline fertility after removal.5 For LARC methods, pregnancy rates range from 0.1% to 0.8% in the first year of typical use.6 Compared to those who use no contraceptive method or short-acting contraceptive methods, people who use LARC are less likely to have short IPIs.7 LARC can be placed immediately postpartum (during the hospital stay) or at an outpatient postpartum visit. The contraceptive implant can be placed at any time following a birth, including during postpartum hospitalization. IUDs are best placed within 10 minutes of placental delivery or at an interval of six to eight weeks postpartum due to the higher risk of expulsion if placed in the interim period.8 Health systems do struggle to obtain reimbursement in many cases when LARC are placed during the delivery hospitalization. Both immediate postpartum LARC and interval LARC reduce short IPIs compared to other forms of contraception or no contraception8; immediate postpartum LARC is associated with the most marked decrease in short IPIs.9
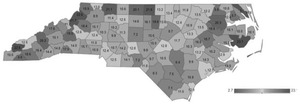
Given that use of LARC decreases the IPI, consideration should be given to strategies that improve access to LARC. In the most recent Pregnancy Risk Assessment Monitoring System (PRAMS) survey data from North Carolina (2019), 16.9% of individuals who had a recent pregnancy were currently using an IUD, and 7.2% were using a contraceptive implant.10 Use of an IUD was more common among White and Latina, more highly educated, married, and non- Medicaid-recipient individuals, while use of the implant was more common among Black and Latina individuals and those with less than high school education, under age 25, not married, and receiving Medicaid.11 NC Medicaid claims data from 2020 indicate that 13% of beneficiaries were using LARC within 60 days postpartum; however, rates varied widely between counties (Figure 1) (NC Medicaid Population Health Impact Brief: April 2022, unpublished data). The majority of this use occurred outside of the immediate postpartum period. While use of LARC is growing in North Carolina, reducing barriers to accessing LARC will likely result in increased uptake and reductions in short IPIs. Barriers to LARC use include cost, limited access to immediate postpartum and same-day LARC placement, and provider education.
Cost
For patients, a major barrier to using LARC can be cost. In the Contraceptive CHOICE study in St. Louis, a prospective study of over 9000 women who received tiered effectiveness counseling on all methods, 75% of participants chose a LARC.12 All contraceptives were available at no cost and available to all patients the day they were in the clinic. In a study among Colorado Title X clinics where LARC devices were available at no cost, the use of LARC increased from 5% to 19% among women aged 15–19 years.13 For low-income patients surveyed in Minnesota, the largest barrier for LARC use was cost.14
Under the Affordable Care Act, most insurance plans, including Medicaid, should offer FDA-approved contraceptive devices to all beneficiaries without cost-sharing.15 In North Carolina, however, given that Medicaid has not been expanded, there are an estimated 400,000 individuals who are not eligible for Medicaid and yet do not have access to affordable private insurance. Fortunately, this gap has been mitigated somewhat for pregnant and postpartum people because, as of April 1, 2022, North Carolina was one of the first states to extend Medicaid to 12 months postpartum, meaning that those individuals who qualify for Medicaid during pregnancy will have uninterrupted coverage for one year after giving birth.16 While this extension increases the number of postpartum people who have coverage for LARC, it does not apply for certain groups. Births covered by Emergency Medicaid only include reimbursement for emergency expenses during birth hospitalizations and do not cover outpatient care or ongoing contraception. Additionally, if a person did not have Medicaid in North Carolina during pregnancy (e.g., because their birth was in another state), they are ineligible for coverage under the postpartum extension.17
Many individuals who are not eligible for full Medicaid after 12 months postpartum will still be eligible for the NC Medicaid Family Planning Program, a limited Medicaid program that fully covers LARC counseling, placement, and surveillance.18 Other programs that help fill the gaps for contraceptive access include the Title X program and 340B medication pricing. In 2019, Title X funded 84 health departments or districts in North Carolina, offering services to patients from all 100 counties.19 Title X programs are required to offer a broad array of contraceptive options, including LARC, to patients on a sliding scale that slides to zero. Typically, patients from households that are at or below the federal poverty level have zero cost, and the proportion of the cost increases to 100% at > 250% of the federal poverty level. Title X funds can cover staffing, infrastructure, and community education services.20 Title X does not cover LARC device costs, but Title X grantees are eligible for 340B pricing and may purchase contraceptive medications and devices at a discount.21 Eligibility for this pricing is limited to a narrow group of safety-net providers including federal grantees from the Centers for Disease Control and Prevention, the Department of Health and Human Services, and the Indian Health Service.22
In addition to patient-level cost barriers, it is also cost-prohibitive for some providers to keep LARC devices stocked in their clinics. It can be challenging to estimate how many devices will be needed during a given time period, and stocking devices that may expire before use is a cost burden that falls on the provider, clinic, or health system and results in devices ordered and never used. VaxCare and Upstream are two programs in North Carolina that can help overcome this issue. VaxCare is a technology platform that improves availability and access to LARC.23 Currently running in North Carolina and Ohio, the system provides LARC inventory for practices on consignment at no cost, automates ordering and inventory management, and bills for the contraceptive device directly using the patient’s medical benefit. The VaxCare technology allows for practices to immediately check insurance eligibility. Stocking the devices and being able to check insurance eligibility in real time facilitates same-day access to LARC and avoids delays related to ordering LARC through specialty pharmacies. Upstream North Carolina is a multiyear initiative that is working to provide sustainable training and technical assistance to health centers to ensure access to all birth control methods and same-day LARC insertions at low or no cost.24 Upstream works with 12 local health departments in North Carolina and is looking to expand its reach.
Access to Immediate Postpartum LARC
To shorten IPIs, it is essential to expand access to immediate postpartum LARC, as not all people are able to access outpatient LARC prior to having an unintended pregnancy. Around half of women report having unprotected intercourse before the routine six-week postpartum visit,8 and the proportion of people who attend their postpartum visit is 72%.25 Among patients in New Mexico who desired an IUD post-delivery, only 60% actually received a device.26 Two major reasons cited were pregnancy prior to insertion and failure to attend the postpartum visit. Immediate insertion of LARC after a delivery likely improves continuation rates and may improve IPIs. In one randomized controlled trial of immediate versus interval IUD insertion performed in North Carolina, more women in the postpartum insertion group were using their IUD six months postpartum (83%) than in the interval placement group (64%).27 In implant users, there has not been a significant difference found with immediate versus interval insertion.28
Potential disadvantages of immediate postpartum insertion of LARC include higher expulsion rates for IUDs (10%–27% versus 2%–7%) and a potential impact on breastfeeding for progestin-containing devices.5,29 For breastfeeding individuals, progestin-containing devices are considered Medical Eligibility Criteria Category 2 (advantages generally outweigh theoretical or unproven risks) until 21 days (implants) and 28 days (IUDs) after delivery due to this potential concern.30 For certain patients, particularly those with poorer access to care, the advantage of immediate postpartum insertion likely outweighs the disadvantages, as one study found that 25% of patients randomized to interval rather than immediate placement did not return for placement of the device.27 ACOG supports the use of immediate postpartum IUD to mitigate barriers to care despite increased risks of expulsion.8
In North Carolina, a major barrier to immediate postpartum LARC is the inability for health systems to be reimbursed for a device placed during the delivery hospitalization. This does not apply to Emergency Medicaid, which applies to approximately 10% of Medicaid births in North Carolina. Each device may cost the health system up to $1200.31 However, since delivery care is typically billed for globally, whether or not a LARC device is placed, the payment for the pregnancy care is the same. Effective October 2018, NC Medicaid introduced new diagnosis-related group codes that could be used for birth hospitalizations including LARC insertion.32 These codes allow for additional cost recuperation to cover the device when a LARC insertion is billed during the delivery hospitalization. Private payers in North Carolina do not offer this option. Therefore, in North Carolina, patients with Medicaid insurance have potentially better access to immediate LARC insertion than those with private insurance.
Health systems handle this differential access differently. Some provide the devices to all and simply do not recuperate the costs for those with private insurance. Some do not provide the devices to any, even those with coverage. Others provide the devices to those with Medicaid insurance only. Interestingly, hospitals get reimbursed the same amount regardless of which LARC is placed. This amount is an average cost of all the devices, weighted for their frequency of use. Therefore, if a patient chooses a less expensive device, the hospital will save money relative to a patient choosing a more expensive device, introducing a potential conflict of interest as to which device may be recommended by health systems and their employees.
Same-Day LARC Access
Availability of same-day LARC insertion is critical for increasing access. When LARC was initially introduced, it was common to require a counseling visit first, followed by a visit on a separate day for placement of the device. This practice decreases uptake, with one study showing that only 50% of Medicaid-insured women who requested LARC returned for the placement visit.33 ACOG has long recommended same-day insertion, and while many practices provide same-day LARC insertion, this service is not universally available. Nationwide, only 35% of health departments and 30% of federally qualified health centers (FQHCs) offer same-day IUD insertions.19 In North Carolina, only 42% of Title X sites offer same-day IUD insertions “always” or “often,” and 52% offer same-day implant insertions “always” or “often,” despite the fact that 21% of their patients at risk for unintended pregnancy choose LARC (2021 NC Family Planning Clinical Assessment Survey, provided by Marissa Peters, Reproductive Health Data Manager for North Carolina Department of Health and Human Services, Division of Public Health, Women, Infant, and Community Wellness Section, Reproductive Health Branch).34 Efforts to increase same-day LARC insertion are necessary to ensure that those who desire LARC are able to receive it.
Provider Education
An important factor in improving LARC access is provider training, as LARC initiation requires a provider trained in placement of these contraceptive methods. Lack of insertion skills can be overcome through trainings provided by organizations including the National Clinical Training Center for Family Planning and the Reproductive Health National Training Center.35,36 Such training directly translates to improved LARC access, especially when combined with funding for contraceptive methods.37
Provider education is particularly important for expanding access to immediate postpartum LARC. While the technical placement of the contraceptive implant is no different from placement at any other time, placing an IUD immediately postpartum does require experience with the postpartum uterus. Both methods require additional knowledge in order to appropriately counsel patients about use in the postpartum period and in the context of lactation. In one study of experienced obstetric physicians, only 42.7% reported experience with immediate postpartum IUD placement, and the most common reason for not having done so was inadequate training.38 Online training for immediate postpartum LARC is available through ACOG’s Postpartum Contraceptive Access Initiative and Partners in Contraceptive Choice and Knowledge.39,40 Beyond the Pill and Upstream both provide virtual trainings on the full scope of contraceptive care, including LARC. The FDA requires manufacturer training for the contraceptive implant, which is available at https://nexplanontraining.com/.
Ethical Considerations
While access to LARC to improve interpregnancy care and reduce the rates of short IPIs is critical, no discussion about LARC can be complete without including the importance of patient autonomy and reproductive justice. Contraceptive counseling at any time must be patient-centered and non-coercive. This is particularly important when discussing postpartum contraception, as public health efforts to increase LARC access and use have been focused on marginalized communities. Those same communities have historically been the focus of eugenics and forced sterilization programs.41 Efforts must continue for increased and equal access to LARC for all, but every discussion of contraception should include all forms of contraception. Implicit bias inevitably contributes to reproductive coercion, and though LARC is effective, it may not be the best choice for each individual. Provider counseling and health care system provision of contraception must take this into account. Moreover, LARC devices are not permanent but often need to be removed by a provider, and access to appointments for removal of devices must be equitable so as to ensure that all patients who desire return of fertility, or to switch to another form of contraception or no contraception, are able to do so within a reasonable time frame.6
Conclusion
Use of LARC methods may lengthen IPIs, and increased use in the population may improve maternal and infant health indicators in North Carolina. Attention should be paid to reducing barriers to access including cost, provider training, and immediate postpartum LARC and same-day LARC insertion, while at the same time being careful to develop policies that are equitable and not coercive, particularly in historically marginalized communities.
Acknowledgments
We appreciate the assistance of Velma Taormina, MD, who reviewed this paper and provided guidance.
Disclosure of interests
No interests were disclosed.