Introduction
Injuries from firearm violence have surpassed motor vehicle crashes as the leading cause of death of children in the United States.1 In addition to these deaths, countless more people are harmed either from injury or as family members affected by the death or injury of a child. It should be noted that although this is a national problem, it is even more significant in North Carolina, as children in North Carolina have a 51% higher risk of dying as a result of a firearm injury than children do nationally.2
Similar to cancer, pediatric firearm death is a complex issue with many different pathologies (e.g., homicide, suicide, unintentional injury) and thus there will not be a single cure nor prevention strategy that is uniformly effective. Instead, a multi-pronged approach is necessary, and following the evidence will save many lives.
While some interventions are community- and policy-based, complementary approaches can occur in the medical setting, especially in the medical home. It has been demonstrated via meta-analysis that providing safe-storage counseling along with firearm-safety devices improves safe-storage rates significantly.3 Unfortunately, this practice is not as widespread as its importance would suggest, as only 7.5% of patient respondents reported even discussing safe storage with their physicians in a 2019 study,4 let alone concomitantly receiving safe-storage devices. Similarly, in a survey of North Carolina physicians, which did not include pediatricians, only 25% reported having conversations about firearm safety “often” or “very often”.5 The relative lack of counseling, which is understandable given other demands on providers’ time, is co-occurring with an increasing number of children nationally being harmed (relative risk 1.9) and causing harm (relative risk 1.43) through increased access to unsecured firearms at the start of the COVID-19 pandemic,6 leading to a substantial (38.8%) increase in pediatric firearm-related hospital encounters.7
According to a modeling study, safe-storage counseling and lock provision have a significant impact on prevention of deaths from unintentional shootings, with models predicting a savings of 72–135 children’s lives per year if there were a 20% increase in firearm-safety counseling.8 There is appetite for improvement in our field, given that 80% of surveyed North Carolina physicians believe that gun violence is a serious health issue and 65% report knowing how to counsel patients about gun safety.5 Despite political tensions that surround this issue as discussed in the media, 75.5% of parents agree that pediatricians should counsel on this topic,9 and as such, primary care pediatricians at Duke Health have been providing counseling and safe-storage devices for over 15 years.
Background
In 2005, Duke Children’s Primary Care (DCPC), in partnership with Jackie Kaufman, a member of the Durham County Health Department Gun Safety Team, approached general pediatric and medicine-pediatric providers with a proposal that they include gun-safety counseling as part of routine well-child checkups (WCC). This initiative was received with polite interest but some degree of hesitancy as well, given the time restraints of fitting in multiple tasks during routine clinic check-ups. There was also some discomfort in addressing a potentially sensitive subject with parents who might be concerned about Second Amendment rights and feel uncomfortable discussing whether there were guns at home. Not to mention that this took place in a political climate that appeared to be less than friendly to clinicians interested in trying to make a dent in the problem of gun violence. Of relevance, on the heels of a similar bill in Florida, in 2015 a bill was brought before the North Carolina state legislature that, if passed, would have made it unlawful for clinicians to ask about gun ownership during doctor visits. Fortunately, this legislative effort to muzzle physicians failed. Despite initial concerns, providers at DCPC soon embraced the incorporation of gun-safety counseling as part of routine “anticipatory guidance” during WCCs. Physician trainees have been especially receptive to embracing this approach.
In the spirit of counseling parents about the importance of using life-saving car seats and keeping poisons and medications locked up at home, discussing gun safety has now become a natural addition to the conversation about keeping kids/teens safe and preventing injuries and deaths. When it is determined that there are guns in the home, the issue of safe storage is discussed, and the offer of free gun locks is made. The adult recipient of the gun lock(s) signs a brief consent form in English or Spanish. To date, the clinical staff at three DCPC clinics have handed out over 1500 gun locks, which have been received with thanks and an acknowledgment that physicians want to collaborate with parents to keep their loved ones out of harm’s way. We see this effort as an alliance with parents who want their kids to stay safe at home as well as in the community and when visiting the homes of friends whose families may own guns. This approach is now spreading to other sites within the Duke Health System, including Emergency Medicine.
Current State
In 2021, the Duke Primary Care network partnered with Duke Children Hospital and Health Center to spread the Firearm Safety Initiative. Duke Primary Care (DPC) is one of North Carolina’s largest primary care provider networks, comprising over 45 primary care and urgent care practices in seven counties across the Triangle area, including Durham, Wake, Orange, Granville, Alamance, Chatham, Vance, and Franklin counties. DPC cares for both children and adults, with more than 200 providers and more than 500,000 patient encounters annually. We started by forming a quality improvement (QI) committee, which decided to launch the Firearm Safety Initiative in WCC visits. Our aims were 1) to increase firearm safety counseling by providers at WCC visits; 2) to increase provider comfort in discussing firearm safety; 3) to increase patient/family awareness of firearm safety concerns; and 4) to distribute free cable gun locks. We selected four general pediatrics and two medicine-pediatrics practices to launch the project. The QI project received exemption from the Duke Health Institutional Review Board.
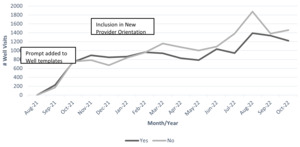
We performed a baseline survey of provider attitudes toward firearm-safety counseling. Not surprisingly, providers expressed some hesitancy about how the counseling would be received by families; providers were also unsure of their skills in delivering the counseling. We then hosted an educational session over lunch for the provider and leaders of the six practices. We also set up an intranet website with educational materials. Free gun locks obtained from the Durham VA were distributed to the practices. Four months later, providers’ confidence in counseling about firearm safety seemed to increase, but it was unclear how much counseling was being done overall. We added a prompt to the electronic health record Well Child note templates used by all providers. The prompt included a trackable “yes or no” element that allowed us to run reports on how often providers self-reported counseling. We also began to include firearm-safety counseling as a talking point during new-provider orientation. In order to reduce administrative burden we did not track the number of gun locks distributed, but due to increasing numbers we had to modify our inventory control process several times.
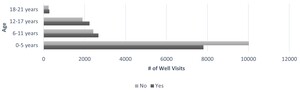
Over the first 15 months of the project, the total number of WCC visits increased after an early nadir due to the COVID-19 pandemic (Figure 1). In the six baseline practices, providers delivered firearm-safety counseling at 13,004 WCC visits for patients aged 0–21 years. This represented 47.1% of total WCC visits at these practices. Counseling was more likely to occur for patients aged 6–21 years than for those aged 0–5 years (Figure 2). Both physicians and nurse practitioners participated in counseling. The QI committee observed that the EHR prompt did not seem to be overly burdensome. Providers felt pride in contributing to lessening the epidemic of gun violence. Families frequently expressed gratitude that we were asking about firearm safety. No negative comments about firearm-safety counseling were recorded in our patient experience surveys. Ultimately, we began encouraging the DPC Family Medicine practices to get involved in firearm-safety counseling.
Conclusion
Our experiences at Duke Health demonstrate that it is practical and feasible to perform firearm-safety counseling and to distribute gun locks in pediatric primary care practice. And yet, primary care pediatricians are only one piece of the puzzle. In order to end the national epidemic of gun violence, we need to advocate for child-access-prevention laws that keep guns out of the hands of children. Pediatricians and other health care providers are important voices in the conversation about firearm-safety policy. The authors have experience advocating for firearm-safety legislation at the state and national level.
Primary care pediatricians can also advocate for expansion of firearm violence prevention within health care settings. Many emergency departments now routinely counsel about firearm safety as part of lethal-means screening. Hospital-based violence interrupter programs partner with community groups to reduce the impact of gun violence; Duke Health launched one such program in 2022. We are also collaborating with mental health professionals and with adult medicine providers to expand counseling to more ambulatory settings. We hope that this discussion serves as a call to action for all health care practitioners in North Carolina to invest their time and expertise in preventing gun violence.
Acknowledgments
We would like to thank our many collaborators: Duke Children’s Primary Care providers, staff, and administration; Duke Primary Care providers, staff, and administration; DPC Firearm Safety Counseling QI committee: Tabitha Smith, DNP, Malinda Teague, Dr. Lisa Ferrari, Dr. Carol Burk; and Dr. Dean Miner for designing the EHR templates; Jackie Kaufman and the Durham County Gun Safety Team; VA Durham Health Care.
Disclosure of interests
The authors report no conflicts of interest.